Peripheral and Central Sensitization
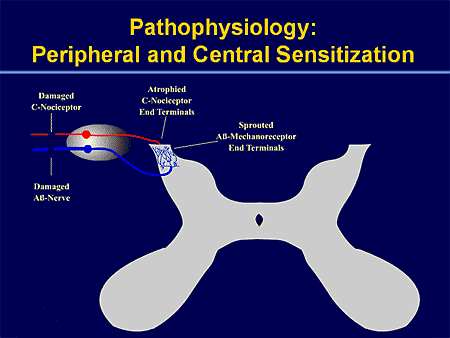
Peripheral and Central Sensitization
Clinical and animal studies provide indirect evidence that the abundance of inflammatory mediators released during migraine have the ability to maintain activation and sensitization of peripheral and central trigeminovascular (TGV) neurons (Noseda & Burstein, 2013). Peripheral sensitization (PS) is an increased sensitivity to innocuous or noxious stimulation by an over Aesponse of primary afferent fibers, causing a throbbing perception. In support of peripheral sensitization, clinical studies have found an increased amount of inflammatory mediators in cephalic venous outflow during migraine, as well as the acute migraine treatment with efficacious NSAIDs (Pietroban & Moskowitz, 2013). In animal studies, in vivo meningeal nociceptor ctivation caused peripheral nerve endings to release vasoactive proinflammatory peptides like CGRP and substance P. These peptides cause neurogenic inflammation which entails meningeal blood vessel vasodilation, localized activation of mast ells from the dura, plasma protein extravasation, and cytokine and other inflammatory mediator release (Pietroban & Moskowitz, 2013). Rat dural nociceptors showed palpable cephalic hypersensitivity as well as long-lasting activation and sensitivity due to dural mast cell degranulation. The process behind PS and inflammation during migraine has not been fully elucidated. About two-thirds of migraineurs experience cutaneous allodynia (CA) in the periorbital region that could spread to extracephalic regions after the onset of headache. CA is pain perception from harmless stimuli and is a sign of central sensitization (CS). Once an inflammatory soup (blend of prostaglandins, potassium, histamine, bradykinin, and serotonin causing hyperalgesia) was applied locally to the dura of anesthetized animals, second order TGV neurons in the TCC displayed greater and longer lasting responses to harmless mechanical or thermal facial skin stimulation (Strassman et al., 1996). Also, third order TGV neurons in the posterior thalamus presented increased and long-lasting responses to whole body skin stimulation. In an fMRI study of migraine patients, innocuous heat and brush stimuli generated a large blood oxygen-level dependent (BOLD) signal in the thalamus of migraineurs showing signs of whole-body allodynia, such as not being able to wear tight clothing or unable to take showers, during a migraine attack versus a pain-free state (Burstein et al., 2010). After chemical stimulation of rat dura, investigators gave an anesthetic block of primary dural afferents which did not prevent long-lasting hypersensitivity to skin stimulation of TCC neurons. This result indicates that CS is independent of afferent input after it has been initiated.


